In Vitro Fertilisation
“I love the fact that my job is on the cutting edge of innovation as far as science goes, and I love being able to help patients achieve the family they want.”
— Dr Myvanwy McIlveen
Let's Explore
What is IVF?
In Vitro Fertilisation, commonly referred to as IVF, is a medical procedure involving the combining of eggs and sperm outside the body, within a laboratory environment.
What are the stages of the IVF journey?
Firstly, you will inject hormonal medications designed to stimulate the ovaries to grow multiple eggs. After 7-9 days of injections we start doing blood tests & ultrasounds every 2-3 days to determine what is the very best day for your egg collection.
We collect the eggs & sperm and then combine them in the lab to make embryos. We can do either IVF or ICSI (intra-cytoplasmic sperm injection). IVF is where we mix the eggs and sperm together in a dish & allow the sperm to fertilise the eggs. ICSI is where we inject one sperm into each mature egg. After successful fertilisation, the embryos are then cultured (grown) for 5 to 6 days in Genea’s special Geri time-lapse incubators.
On day 5 we choose the best quality blastocyst for transfer. The embryo transfer is similar to having a pap smear. If available we will freeze any extra good quality embryos allowing us the option of a baby brother or sister in the future. Eight days later we do a pregnancy test to see if implantation has occurred.
“Do you know using the GROW App you can receive images of your embryos developing in the lab during your IVF cycle?”
– Dr Erin Fuller
What are the advantages of IVF?
IVF increases the chances of having a baby for the vast majority of causes of infertility including PCOS, male factor sperm issues, tubal disease, unexplained infertility and endometriosis. By helping with fertilisation, selecting the best embryo and putting it directly inside the uterus we see a big increase in pregnancy rates.
When is IVF the optimal choice?
- When other treatments have failed
- When you have been trying for a long time
- When you are 38 years or older (time isn’t our friend)
- Low sperm count
- Blocked tubes
What are the risks and side-effects associated with IVF?
While IVF is a generally safe procedure, the hormonal medications administered for ovarian stimulation can lead to side effects such as mood swings, bloating, and discomfort. The egg retrieval process carries a small risk of bleeding, infection, or accidental damage to surrounding structures. IVF can also be stressful- our counsellor is available for support should you need her.
“We’ve been providing IVF services for our patients for over 30 years. We’ve been at it so long that their babies are having babies!”
— Dr Myvanwy McIlveen
What’s the typical IVF duration?
How long does it take to do IVF? The duration of an IVF cycle can vary; however, it is usually 4-6 weeks. This timeline includes ovarian stimulation, egg retrieval, fertilisation, embryo culture, and embryo transfer. Additional time may be needed for pregnancy testing and follow-up appointments. Various factors, including the specifics of the treatment plan and your menstrual cycle influence how long each cycle takes.
What’s the process for egg and sperm collection?
An egg collection involves placing a thin, ultrasound-guided needle, through the top of the vagina and into the ovaries. Your doctor then aspirates fluid from the follicles housing the eggs. This procedure is typically performed using sedation in a procedure room at Genea. You are admitted to Lingard hospital to recover afterwards. Some patients opt for or are advised to have a general anaesthetic (fully asleep). Your partner or a support person is welcome to be in the procedure room with you as long as you are not having a full anaesthetic.
On the same day we collect eggs we need a sample of sperm. If your partner is providing this they will be asked to self collect at home or at the clinic that morning typically just after the eggs are collected. In situations where a surgical sperm retrieval is required, we can do a testicular sperm extraction (TESE) or epididymal sperm aspiration (PESA). We do these with sedation, pain relief & local anaesthetic.
Once both eggs and sperm are collected, they are prepared for fertilisation in the lab by a skilled embryologist who assesses sperm quality and selects the most optimal sperm for the fertilisation process. All procedures adhere to stringent medical, identification and ethical standards.
How does IVF address my infertility concerns?
Which lifestyle factors influence IVF suitability?
Maintaining a healthy body weight, stopping smoking, regular exercise and prenatal vitamins all help. Some people find stress management techniques such as yoga, mindfulness and/or meditation helps their mental health during what can be a stressful journey. But don’t stress about stress- it does not have an impact on success rates!
IVF Success
What are the IVF success rates?
IVF success rates are dependent upon lots of factors, including age, general health, underlying causes of infertility, and lifestyle factors. Generally, younger individuals have higher success rates, with success rates ranging from 50% per attempt for women under 30 to 30% for women aged 39-42 years. Age more than any other factor influences your chances of success but also being healthy & choosing the IVF clinic with the best success rates will help.
Here are the IVF success rates for our IVF clinic, Genea Newcastle:
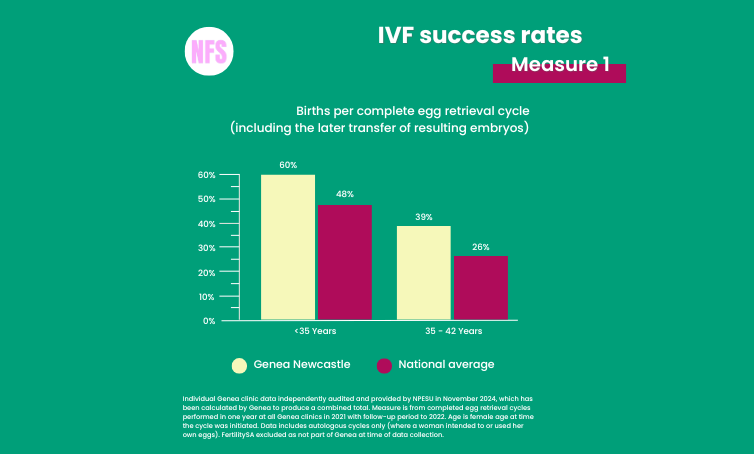
If you’d like to compare you can search for any clinic’s IVF success rates at this website established by the Australian Federal Government: https://yourivfsuccess.com.au/clinics
What does Genea do to help you?
Did you know that at Genea you can watch your embryos GROW?
Using the GROW App images are shared from the GERI incubator to your phone each day allowing you to watch your embryos develop in the lab. You can even try & guess which embryo the lab is going to choose for transfer!
What are my financial considerations?
The cost associated with IVF may vary, ranging from approximately $4,500 to $12,500 out of pocket per stimulated IVF cycle, depending on Medicare, health insurance, the safety net & the NSW government IVF rebate. For most people it is around $4500-$9500 out of pocket for your first cycle. This includes everything apart from some prescription fees (usually less than $200). A frozen embryo transfer will cost between $2700-$4000 depending on your circumstances.
Male Fertility
& ICSI
How does Intracytoplasmic Sperm Injection (ICSI) work?
ICSI is a common part of IVF, particularly when male fertility issues such as low sperm count, poor sperm motility, or abnormal sperm morphology are evident. Additionally, individuals who have experienced poor fertilisation during IVF may opt for ICSI to enhance fertilisation rates.
Can I freeze sperm?
We often use frozen sperm during an IVF cycle for various reasons including remote work, concerns about performance or previous cancer treatment.
How long can you freeze sperm for IVF?
Typically, it can be safely stored for many years with good success rates.
Endometriosis
& IVF
What is endometriosis?
Endometriosis is a chronic condition where tissue similar to the uterine lining grows outside your uterus, causing pain, menstrual irregularities, and potential blocked fallopian tubes
Is IVF recommended if I have endometriosis?
Yes. Endometriosis can lead to pelvic scarring, tubal damage, and reduced egg quality, hindering natural conception. IVF bypasses the effects of endometriosis by directly fertilising eggs outside the body and transferring your resulting embryos into the uterus, increasing your chances of pregnancy.
Genetic Testing
& IVF
Do I need genetic disease screening?
For individuals harbouring concerns about inherited genetic diseases, Non-Invasive Prenatal Screening (NIPS) offers a non-invasive option. This diagnostic tool analyses cell-free DNA extracted from the bloodstream to assess the risk of specific genetic conditions, such as Down syndrome, in the developing foetus.
How useful is Preimplantation Genetic Diagnosis (PGD)?
Another valuable tool is Preimplantation Genetic Diagnosis (PGD), which entails the screening of fertilised embryos prior to their implantation in the uterus. This process enables the identification of genetic disorders or chromosomal abnormalities. For individuals with known genetic risks or a history of specific disorders, PGD presents the opportunity to select embryos devoid of such conditions, thereby reducing the risk of transmitting them to offspring.
What are the benefits of Non-Invasive Prenatal Screening (NIPS)?
Low Risk: NIPS entails a straightforward blood draw from the arm, eliminating the need for invasive procedures, thereby reducing associated complications and miscarriage risks.
High Accuracy: NIPS exhibits commendable accuracy in detecting certain chromosomal abnormalities, surpassing traditional screening methods. This results in a reduced incidence of false positives and false negatives.
Early Detection: NIPS can be conducted as early as the 10th week of pregnancy, affording ample time for informed decision-making.
